I’ve never been one to ask myself the “why me” question when something doesn’t go as planned in my life. Thankfully, when times have been difficult I’ve been able to skip past this question and look for solutions by asking “what if”. Often, when life presents a...
Health & Wellness
We’ll help you find ways to improve your wellbeing in everything you do—from daily meals to sleep. Whether you’re looking for tips on managing stress, mental health or something else, our resources and health experts make sure you get the most out of life.
How to Deal With Big Changes in Your Life
The one constant in life is change. One might get a new job, have a baby, graduate or move to a different city. Even though changes can be exciting, they can also be stressful. My patients frequently ask for coping strategies to deal with the big changes in life. Here...
Safe Sleep Practices for Newborns
Welcoming a baby into the world is a happy and exciting time! One of the most important aspects of caring for a baby is ensuring safe sleep. Infants typically sleep 16 to 18 hours a day, which is essential for their growth, development and overall health. Safe sleep...
Could an Ongoing Cough or Chest Cold Be Asthma?
I often see patients in my office who are dealing with a cough or chest cold that won’t go away or returns repeatedly. With these symptoms, I consider if my patient might have asthma.
Heart Rates: What’s Normal, What’s Not
As a cardiac electrophysiologist, my specialty is treating heart rhythm concerns. This could be a heart rate that is too slow, too fast or irregular. Let’s learn more about what your heart rate means and when to be concerned. What Does Your Heart Rate Measure and Why...
What Is Vertigo and How Is It Treated?
Imagine a sudden feeling of spinning when you first get out of bed that makes you feel like you’re on a carnival merry-go-round that won’t stop. You feel clammy, nauseous and out of control.
Making Waves: The Benefits of Aquatic Therapy for All Ages
Do you have aches and pains? Want to move easier? Interested in ways to improve your child’s strength and balance? Whatever goal you may have for yourself, your child or a family member, there are different ways aquatic therapy can help. What is Aquatic Therapy?...
10 Tips for Parenting with Love, Structure & Flexibility
Parenting is one of the most fulfilling yet demanding roles you can take on. Over the years, through my professional experience and my own journey as a parent, I’ve realized that perfection isn’t just unattainable—it can actually get in the way. Let me share a few...
Navigating Life with Migraines: My Journey and Insights
Have you ever felt a headache so overwhelming that it seemed to take over your entire day, leaving you desperate for relief? For me, migraines became an unwelcome companion during high school. Back then, I didn’t even know what to call them; I just knew that the...
Get the Protein You Need: How Much & What Kind Is Best for You
As a doctor, I get a lot of questions about how much protein we actually need. There is so much information available to us that finding the “right” answer can be hard. Protein is an important part of a well-balanced diet. However, getting the correct amount is just...
Holiday Season Self-Care for Moms
For my kids, it’s truly the most magical time of the year! For me though, as a mom, it’s also the season of heightened mental load and sensory overload. I feel the weight of planning, coordinating and making sure every moment is brimming with holiday cheer. I want my...
How to Lower Your Cholesterol
Do you have high cholesterol? Or have you been told to watch your cholesterol level? You might wonder what steps to take. Eat healthier, maybe more veggies? Exercise more? Limit calories? So many questions! I hope to help provide a little direction to help you. What...
Breast Cancer & Lymphedema
Lymphedema is a condition that occurs in one in five breast cancer patients. It might occur right after surgery or radiation therapy, or it might happen months or years later or not at all. If lymphedema is not treated, it can become debilitating and cause an...
Knee Pain & Surgery: How to Avoid It & When to Know It’s Time
If you’re experiencing knee pain, you might be wondering what you can do to avoid surgery and when surgery might be your best option. Here are answers to these common questions and information to help you determine next steps to resolve your knee pain. Knee Pain, Why?...
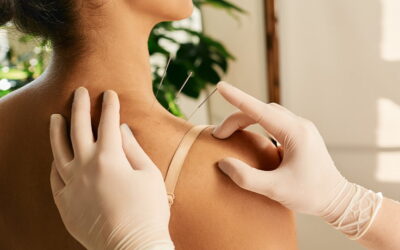
Acupuncture: Ancient Medicine with Modern Applications
My interest in acupuncture started while working alongside an acupuncturist in Anchorage, Alaska, at a large medical clinic. I was working as an X-ray technician, massage therapist and laboratory technician. I was also experiencing chronic neck pain due to a...
Building Better Bedtime Routines
Hi, I'm Ashley. And I'm Rachel. Welcome to our series, CapitalMOM Real Life Conversations. This week, we're going to be talking about bedtime routines—how they're different for every family, but ultimately how we use this time to connect with our children in different...
Preparing for a New Family Member
3,591,328—the number of babies born in the U.S. in 2023. Wow! That’s a lot of homes adding a new family member. And what about the 1 in 25 U.S. families who have at least one adopted child? Or the six million U.S. households that have more than three generations...
8 Tips to Avoid Injury: Insights from Sports Medicine Trainers
Whether you’re a weekend warrior, a recreational sports enthusiast or professional athlete, we can all use tips to avoid injury and stay healthy. We asked our athletic trainers to share some of their best tips.1. Listen to Your Body & Address Pain or Discomfort...
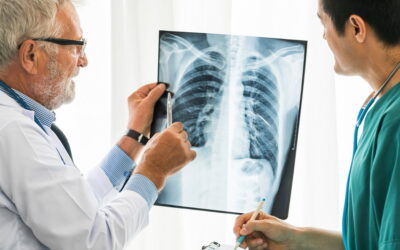
New Advances in Care: What Do I Need to Know If Someone I Love Is a Past or Current Smoker?
We all know it — smoking is not good for you. Yet for many, it is a reality of our daily lives. Let’s face it, it’s addictive and it’s often not easy to stop. And some people don’t want to quit. Given all of this, what’s a person to do? What steps can you take to make...
How to Avoid Burnout in Work & Life
Do you feel sluggish and exhausted? Can simple tasks seem overwhelming to complete? Have you found yourself so stressed out that you quickly become angry or frustrated? If you’ve noticed feeling this way, you might be experiencing burnout. Burnout can be difficult to...
Let’s Talk Osteoporosis: How to Keep Your Bones Strong
It might seem hard to believe but we reach our peak bone mass in our late 20s or early 30s. From there, men and women start to lose some amount of bone density throughout their lifetime. The loss in bone density causes an abnormal structure and ultimately weakens our...
Multiple Sclerosis and Dietary Changes
As a neurologist and subspecialist in multiple sclerosis, I am dedicated to helping patients with MS live their best lives. Many patients have questions about how dietary changes can impact their life. You will find that a well-balanced diet fuels your body and...
Six Common Ways We Struggle During Holidays
Elvis once sang about feeling blue at Christmas time, and I’m here to tell you: It’s perfectly normal to feel that way. There are many reasons why your days may not be merry and bright around the holiday season. Jam-packed social calendars, deadlines at work, loss of...
Straight Talk on Mammograms and Breast Cancer
The primary focus of most women is not themselves. Women for the most part are focused on taking care of their family and put themselves at the bottom of the list. It is time to change this way of thinking and put you and your priorities at the top of your list! You...
Boundaries for Mental Well-Being
Boundaries are limits we set between ourselves and others. They are separations that humans need to feel safe, valued and respected. Understanding the various forms of boundaries, recognizing when it’s time to set boundaries and learning how to set boundaries...
Don’t Let Balance Issues Hold You Back
Now is a great time to get out and enjoy opportunities for fun. Maybe it is a walk in the park, looking around and enjoying the birds and nature. Or it may be watching your child or grandchild’s soccer game or even playing lawn games like bocce ball at home! Or maybe...
A Parent’s Guide to Infant, Baby & Toddler Sleep
Sleep—the one thing new parents are always deprived of themselves. But what about our little ones? How can we keep them safe and ensure they are getting enough sleep in the optimal environment? It starts when you bring your baby home. What to Expect After Bringing...
Summer Eye Safety
For many families, summer is the most wonderful time of the year. School is out, days are long, sun is plentiful and vacations, cookouts and family time outdoors are common. Here are four tips to keep your eyes safe during this summer season. Avoid Getting a "Sunburn...
Supporting Positive Mental Health in Your Child
Recent data released from the Centers for Disease Control & Prevention (CDC) shows that one in four high school students are feeling persistently sad and hopeless, and nearly one third are struggling with poor mental health. As a child and adolescent psychiatrist,...
Exercise Is the Best Way to Manage Arthritis Pain
Your knees, hips or back are stiff and sore and sometimes hurt with certain movements, so why would you want to strength train or do other types of exercise? Simple: Exercise is crucial for people with arthritis of all kinds because it: Increases strength and range of...
Use Our Symptom Checker
Whether it’s a rash, your child’s ear pain or your aching back, our symptom checker can help determine what to do. Just answer a few questions about your symptoms and receive recommendations for care.
Find a Doctor
Find the right provider for you. Search by specialty, view provider videos and even schedule an appointment online. Life’s busy, we make finding a provider fast and easy to fit your schedule.
Stay Informed for Your Health
You and your family are unique. At Bryan Health, we have a variety of classes, events, podcasts and more for all stages of life.
To stay in the know, subscribe to our monthly For Your Health email!
Tune in to…Bryan Health Podcasts
Our 10-minute podcasts provide practical, useful advice for a lifetime of good health.
And they’re easy to listen to while you’re on the go, at work or at home. Listen to or download a free podcast today!
Register for the Bryan Baby App
Access pregnancy, childbirth and newborn care resources anytime, anywhere.
The Bryan Baby App includes the tools and support you need at every stage of your pregnancy journey and beyond.